What is cancer?
Our bodies are made up of millions of cells. They constantly replace worn out cells with new ones to keep us healthy or when we hurt ourselves (for example, get a cut or graze).
When our body destroys an old cell, one of the remaining cells will make a copy of itself by splitting into two, replacing the old cell. This process is usually carefully controlled so that the number of new cells created is the same as the number that were destroyed.
But sometimes cells can't respond to the signals that tell it to stop dividing. The cell divides again and again, making more and more copies of itself. This eventually forms a lump called a tumour. When a tumour grows uncontrollably and invades surrounding tissues or spreads further away, this is known as cancer.
Tumours
A tumour (also known as a neoplasm) is any abnormal mass of tissue (collection of cells). Like a cyst, a tumour can form in any part of the body. A tumour can be benign (non-cancerous), malignant (cancerous) or borderline (between malignant and benign).
Benign tumours may cause symptoms. But in most cases they don't come back after surgical removal (having an operation).
Malignant tumours are made up of cells that grow out of control. Cells in these tumours can invade nearby tissues and spread to other parts of the body.
Sometimes cells move away from the original (primary) cancer site. Cells spread to other organs and areas through the bloodstream or the lymphatic system (tiny vessels similar to blood vessels passing clear fluid towards the heart). They can continue to grow and form another tumour at that site. This is known as metastatic or secondary cancer. Metastases keep the name of the original cancer location. So ovarian cancer that's spread to the liver is still called ovarian cancer and is different from a cancer that starts in the liver.
Borderline tumours are rare types of tumour growth. Although the cells look abnormal they rarely grow out of control.
To find out whether a cyst or tumour is benign or malignant, a sample of the affected tissue – or in some cases the entire suspicious area – is removed and studied under a microscope. This is known as a biopsy.
Ovarian cancer
The ovaries are two small organs, each about the size and shape of an almond. They’re located low in the tummy area called the pelvis, just behind the pubic area. They form part of the female reproductive and hormonal systems, storing a supply of eggs.
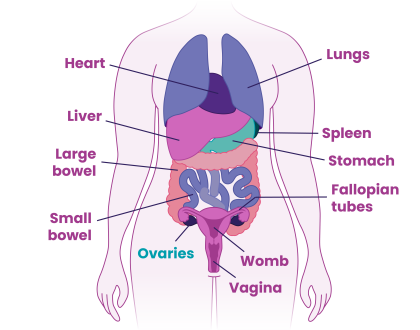
Each month an egg is released from one of the ovaries through the fallopian tubes into the womb ready for fertilisation (when sperm and an egg joins together). The ovaries also make the female hormones oestrogen and progesterone.
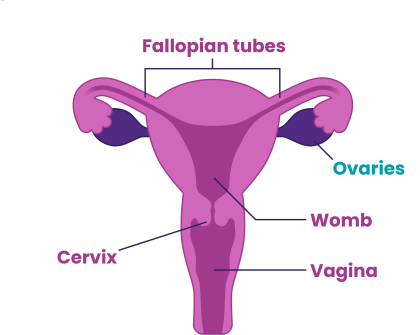
Ovarian cancer starts from the cells in and around the ovary and fallopian tubes. There are many different types of ovarian tumours classified by the types of cells and tissue they start from.
Ovarian cancer metastases (secondary cancers) are lumps formed in other parts of the body because of the spread of ovarian cancer cells.
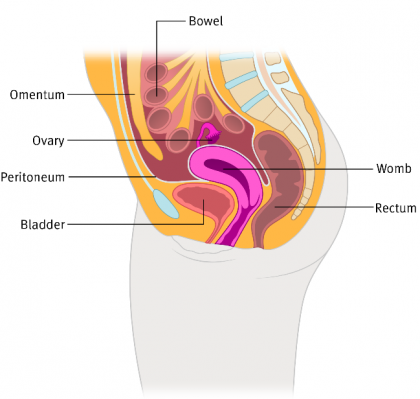
Ovarian cancer cells tend to spread on the lining of the tummy (abdomen) called the peritoneum (a large, thin, flexible sheet of transparent tissue that covers the organs inside your abdomen). They often form lumps on the surface of the bowels, the omentum (a fatty layer of tissue that extends downwards from the stomach) and the surface of the liver. They can form lumps within the liver, the spleen or the lungs but this is rare. These lumps (metastases) often produce excess fluid in the tummy called ascites, which can cause significant bloating and uncomfortable symptoms.
Understanding the type of cancer (the histological type), if and how it has spread (the stage), and how different the cancer cells look compared to normal cells (the grade) can help you when discussing your diagnosis, treatment and prognosis with your specialist. But you may not wish to know so much detail – it's a personal choice.
Last reviewed: April 2022
To learn more about our review process, take a look at our information standards.



